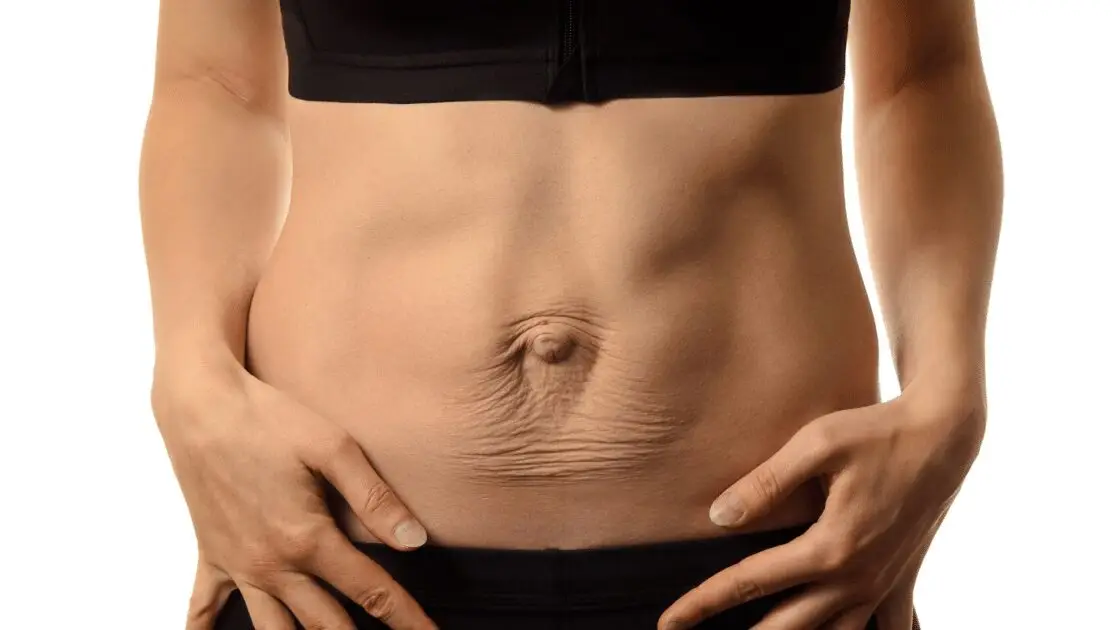
Understanding and Preventing Diastasis Recti (Abdominal Separation)
If you are currently pregnant you may well have been reading up

If you are currently pregnant you may well have been reading up

By Kayden Wu (M. physio) Introduction: An Anterior Cruciate Ligament (ACL) tear

Weightlifting has become a popular form of exercise in recent years, with
Be Inspired
Be Informed
Reach Your Goals
